 by Carolyn Thomas ♥ @HeartSisters
by Carolyn Thomas ♥ @HeartSisters
Turns out that the kind of heart attack that I had (caused by a 95% blockage in the big left anterior descending coronary artery) – the so-called widowmaker heart attack – may actually be relatively uncommon in women. You might guess that fact by its nickname. It’s not, after all, called the “widower-maker”.
While cardiologists warn that heart disease can’t be divided into male and female forms, there are some surprising differences. Cardiologist Dr. Amir Lerman at the world famous Mayo Clinic in Rochester, Minnesota, told the Los Angeles Times recently:
“When it comes to acute heart attacks and sudden death from cardiac arrest, women have these kinds of events much more often without any obstructions in their coronary arteries.”
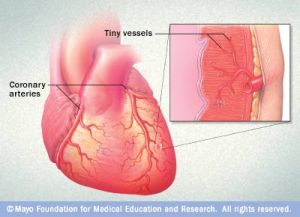
Instead, it appears that a significant portion of women suffer from another form of heart disease altogether. It affects not the superhighway coronary arteries but rather the smaller arteries, called microvessels. These tiny arteries deliver blood directly to the heart muscle.
Ironically, I can now boast two diagnoses for the price of one – first, the widowmaker heart attack caused by a fully occluded coronary artery back in 2008, and then, after several months of puzzling, ongoing cardiac symptoms – like chest pain, shortness of breath, and crushing fatigue – a second diagnosis of inoperable coronary microvascular disease. Continue reading “How women can have heart attacks without having any blocked arteries”