 by Carolyn Thomas ♥ @HeartSisters
by Carolyn Thomas ♥ @HeartSisters
In 2018, many viewers of the hit NBC television drama “This Is Us” learned the term “widow maker heart attack” for the first time when the beloved main character Jack Pearson was pronounced dead. As TIME magazine later reported, online searches for that term spiked more than 5,000 per cent in the hours after that episode aired. Some viewers took to social media to tell their stories about loved ones who had died from – or survived – their own cardiac events.
Television is so educational! .
I didn’t hear the words “widow maker” until my first follow-up appointment after my own heart attack. My doctor reviewed my latest cardiac test results and then calmly told me that the type of heart attack I’d just survived is what doctors call the “widow maker”. If I hadn’t already been in an extreme state of post-heart attack stun at that time, I’m sure those words would have sent me there.
The name seems pretty straightforward, implying that a man diagnosed with a widow maker heart attack doesn’t usually survive, thus making his wife a widow. But please note, of course, the inherent gender bias on full display here: when women like me experience this heart attack, do doctors call it the “widower-maker”? NO, they do not.
In other words, it’s been historically considered a male heart attack, with a male heart attack name.
As interventional cardiologist Dr. Gary Niess explained:
“The ‘widow maker’ is a lay term for a particular type of heart attack. Any artery closure can cause a heart attack where the heart muscle dies, but the ‘widow maker’ has a higher rate of mortality.”
A widow maker can happen when you develop a big blockage in one of the big coronary arteries that feed the heart muscle – big enough to block all or most blood flow to that muscle. If untreated, this can make the heart stop beating normally, increasing the risk of a deadly cardiac arrest.
As alarming as the ‘widow maker’ name may seem, it’s important to remember that the majority of heart attacks are NOT fatal, as retired professor of medicine, author and cardiologist Dr. Richard Fogoros reminds us:
“Studies have found that survival rates for people hospitalized for heart attacks are approximately 90-97 per cent. This varies based on the type of heart attack, which arteries are involved, and factors like age and gender.”
We also know that acute heart attack survival rates are generally improved if patients seek immediate medical help when early cardiac symptoms strike. Blocked coronary arteries during a heart attack can be unblocked (or “revascularized”) typically via angioplasty, an implanted stent, or coronary artery bypass graft surgery. There is solid research evidence that opening a severely blocked artery during an acute heart attack lowers the risk of death, further damage to the heart, and future heart failure.
Two arteries in particular can be the culprits here: the Left Main coronary artery or the Left Anterior Descending coronary artery (LAD). As Dr. Fogoros adds:
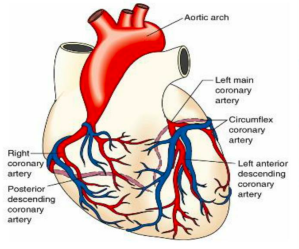
And here’s how Cleveland Clinic critical care cardiologist Dr. Penelope Rampersad describes the LAD (the culprit artery in my own heart attack):
“This artery delivers a major amount of blood to your heart. Because it serves such a big portion of the heart, the LAD artery is a particularly dangerous place to get a clot. A lot of damage can be done to the heart muscle if blood flow isn’t restored quickly. If there’s no blood flow to the heart, the heart muscles become deprived of oxygen and vital nutrients, and heart muscle damage starts immediately.”
A widow maker heart attack is also associated with an increased risk of heart failure and stroke.
Dr. Stanley Chetcuti, who is an interventional cardiologist at the University of Michigan, explains the widow maker heart attack:
“When underlying cholesterol and plaque in your coronary artery comes into contact with the bloodstream, the vigorous reaction creates blood clots. You could go from a 20 per cent blockage to 100 per cent instantaneously.
“A patient experiencing a widow maker would have typical heart attack symptoms of chest or arm pain, lightheadedness or shortness of breath, among others. It’s not different from any other heart attack – it’s just in a more critical area. Immediate treatment is key.
““The quicker you come to the hospital, the better. If you suspect you’re having a heart attack, it’s critically important to call 911.”
♥
NOTE FROM CAROLYN: I wrote about surviving a misdiagnosed widow maker heart attack – and much more! – in my book, A Woman’s Guide to Living with Heart Disease. You can ask for it at your local bookshop or library, or order it online (paperback, hardcover or e-book) at Amazon – or order directly from my publisher, Johns Hopkins University Press (use the JHUP code HTWN to save 20% off the list price).
.
Q: Should the “widow maker” name still be used?

I, like you, had not heard the term “widow maker” until my first after-event appointment with my cardiologist. However, when he said it, I immediately replied, “No, that’s wrong. Call it a widower-maker for me.”
He looked at me like he didn’t get it – and didn’t respond. I don’t think he did get it!
LikeLiked by 1 person
Oh my. . . I suspect you are right, Jane. He probably did NOT get it. . . It’s bad when you have to explain the bleedin’ obvious to otherwise intelligent educated people!
Take care, stay safe. . . ♥
LikeLike
Words are very powerful. Terminology such as “widow maker” and “heart failure” strike unnecessary fear in the hearts of those who hear them. Both these terms need to be retired.
However, until the majority of cardiologists decide that, what their clients hear, is as important or more important, than what they have to say…..
There is likely little motivation to take on the task.
Blessings!
LikeLiked by 1 person
I agree, Jill. I’ve been lobbying cardiologists at every opportunity for years to change the name “heart FAILURE“ – words that are so caustic and damaging when aimed at a freshly-diagnosed heart patient, with almost hilarious responding excuses for NOT changing the name (e.g. “I always use ‘air quotes’ when I say the words ‘heart FAILURE’ to my patients so they know I don’t really mean that their heart is FAILING…” – which is an utterly preposterous statement.
What other medical diagnosis requires AIR QUOTES to soften the blow of hurtful words? And if FAILURE is not what you mean, then STOP SAYING IT!
One cardiologist who was leading a Heart Failure Conference responded to my request like this: ‘Changing the nomenclature at this time is unlikely’ which I thought was a hilariously apt response. People who use words like ‘nomenclature’ to patients apparently can’t see anything wrong with saying ‘your heart is FAILING’ either!
Take care, stay safe. . . ♥
LikeLike
Your story about “air quotes” gave me a chuckle. As a nurse I was CONSTANTLY explaining to patients and families that Congestive Heart FAILURE did NOT mean the heart was truly “failing”.
And now, what I have is referred to as “Heart Failure with Preserved Ejection Fraction”
How many patients who are not cardiac nurses would even understand that??
Maybe we could develop a translation app for cardiac terminology – LOL
LikeLiked by 1 person
Absolutely true! Not many patient who are NOT cardiac nurses (or docs) would have a clue what your own diagnosis means when they first hear it. I did include “Heart Failure with Preserved Ejection Fraction” in my patient-friendly, jargon-free glossary here.
Still, medicine is so jargon-heavy that it’s challenging to be able to translate! I just try to break it all down into small digestible chunks.
♥
LikeLike