 by Carolyn Thomas ♥ @HeartSisters
by Carolyn Thomas ♥ @HeartSisters
Turns out that the kind of heart attack that I had (caused by a 95% blockage in the big left anterior descending coronary artery) – the so-called widowmaker heart attack – may actually be relatively uncommon in women. You might guess that fact by its nickname. It’s not, after all, called the “widower-maker”.
While cardiologists warn that heart disease can’t be divided into male and female forms, there are some surprising differences. Cardiologist Dr. Amir Lerman at the world famous Mayo Clinic in Rochester, Minnesota, told the Los Angeles Times recently:
“When it comes to acute heart attacks and sudden death from cardiac arrest, women have these kinds of events much more often without any obstructions in their coronary arteries.”
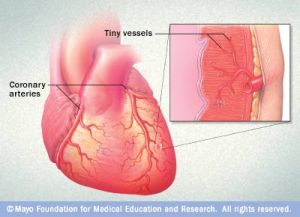
Instead, it appears that a significant portion of women suffer from another form of heart disease altogether. It affects not the superhighway coronary arteries but rather the smaller arteries, called microvessels. These tiny arteries deliver blood directly to the heart muscle.
Ironically, I can now boast two diagnoses for the price of one – first, the widowmaker heart attack caused by a fully occluded coronary artery back in 2008, and then, after several months of puzzling, ongoing cardiac symptoms – like chest pain, shortness of breath, and crushing fatigue – a second diagnosis of inoperable coronary microvascular disease.
In 2006, research published in the journal Circulation looked at the Women’s Ischemia Syndrome Evaluation (WISE) study data on almost 1,000 women referred for cardiac testing due to their symptoms(1). Here’s what they found:
- 62% had non-obstructive coronary artery disease – defined as blockages less than 50% of the artery
- 17% had one coronary artery vessel significantly blocked or narrowed
- 11% had two vessels narrowed
- fewer than 10% had three vessels affected
Dr. Noel Bairey Merz, a cardiologist at Cedars-Sinai Medical Center in Los Angeles, headed up the WISE study, which began in 1996. The average age of her participants was 58, but a quarter were younger and pre-menopausal.
Researchers found that what’s known as ischemic heart disease (any decreased blood flow and oxygen to the heart muscle) is often caused by a blockage within one or more coronary arteries that are feeding the heart muscle, but can also be due to at least two other possibilities:
- dysfunction of the smallest coronary microvascular arteries
- coronary spasm
1. Coronary Microvascular Disease
They used a test in which doctors first measured blood flow through the heart and then injected a drug that should have made the arteries dilate and increased the flow. If the flow did not rise, the patient most likely had microvascular disease.
One third of the women in the L.A. study had low blood flow to the heart muscle caused by coronary microvascular disease. For these women, the rate of deaths or heart attacks was higher than would be expected for other women with normal angiograms.
According to the Texas Heart Institute, coronary microvascular disease most likely happens when small blood vessels in the heart tighten or constrict. This tightening reduces the blood flow to the heart muscle and causes the pain of angina pectoris (a Latin phrase that means “strangling in the chest“).
The encouraging news at first: because these vessels are so tiny, early research suggested that they may not increase the risk of a heart attack or death. But the Journal of the American Medical Association reported in 2005 that the prognosis of patients with unstable angina and non-obstructive coronary artery disease is not benign and includes a 2% risk of death or heart attack at 30 days of follow-up(2). (JAMA. 2005;293(4):477-484. doi: 10.1001/jama.293.4.477)
Problematically, coronary microvascular arteries are too small to detect with the standard cardiac tests that cardiologists would normally use to see larger vessels, so women in particular are often dismissed and sent home with a misdiagnosis in spite of severe and distressing cardiac symptoms.
For example, in typical patients with coronary artery disease, coronary angiography – considered the ‘gold standard’ of cardiac diagnostics – usually shows a clearly blocked artery that slows blood flow to the heart muscle.
But in patients with coronary microvascular disease, these test results are normal – even though symptoms may be as debilitating as those experienced during a heart attack.
Dr. Noel Bairey Merz adds that angiograms that would clearly spot blockages in major heart arteries can miss coronary microvascular disease altogether. As a result, many women who have gone to their doctors with chest pain have gone home with a clean bill of heath – and most likely feeling very embarrassed for having made a fuss over nothing. She says:
“Historically, women have been told that it was in their head.”
According to the Harvard Heart Letter, the preferred diagnostic tool for correctly identifying coronary microvascular disease is coronary reactivity testing.
“Coronary reactivity testing is an angiogram-like test lasting 60 to 90 minutes; it allows doctors to see how very small vessels supplying the heart respond to different ‘challenges’ from medications. “
Texas Heart Institute experts tell us that up until recently, the only treatment for coronary microvascular disease (also sometimes known as Cardiac Syndrome X, a name that’s generally hated by those of us diagnosed with MVD because of its implication that this disorder somehow doesn’t exist!) has been with these medications:
- Nitroglycerin (nitro) can widen or dilate the arteries and improve blood flow to your heart. Nitro can be given through a skin patch, pills, an ointment, or a spray. See more on nitroglycerin.
- Beta blockers “block” the chemical or hormonal messages sent to your heart. When you are under physical or emotional stress, your body sends signals to your heart to work harder. Beta-blockers block the effect these signals have on your heart, so they reduce the demands on your heart.
- Calcium channel blockers can help to keep your arteries open and reduce your blood pressure by relaxing the smooth muscle that surrounds the arteries in your body. The oxygen demand of the heart is also reduced by these medicines.
Physical exercise has also been shown to be helpful in managing MVD symptoms. A Swedish study reported in the Journal of the American College of Cardiology in 2000 suggested that being out-of-shape is a “prominent feature” in patients diagnosed with MVD. Researchers found that a 30-minute workout on an exercise bike three times a week resulted in increased exercise capacity with lesser chest pain for the MVD patients they studied.
As more physicians become educated about the widespread incidence of coronary microvascular disease, particularly in women patients, more treatments are becoming available, including my own particular current treatment for microvascular disease: wearing a portable TENS machine all day long to help increase blood flow to the heart muscle and thus reduce chest pain symptoms. Read more on this underused, non-drug, non-invasive cardiac treatment in “My Love-Hate Relationship With My Little Black Box”.
And emerging research has shown significant success using TENS neuromodulation to treat the chest pain of angina. In fact, the U.K. National Refractory Angina Group now recommends TENS therapy for the debilitating chest pain of angina:
“Neuromodulation owes its origins to Melzack and Wall’s gate theory of pain that predicted that stimulation of vibratory afferent nerves would reduce or gate the transmission of pain traffic relaying through the spinal cord at the same point.
“Transcutaneous electrical nerve stimulation (TENS) was specifically designed to make use of this predicted effect and was used to treat a variety of pain conditions before it was shown to be effective in angina.
“TENS neuromodulation should be offered as part of a multidisciplinary angina management programme based on the current guidelines.“
2. Coronary Spasm Disorders
Another example of non-obstructive heart disease often seen in women is called Prinzmetal’s Variant Angina, chest pain caused by a spasm of a coronary artery. While Prinzmetal’s is not thought to cause a heart attack, chances of a cardiac event are higher in those with underlying heart conditions.
We don’t yet know exactly what causes coronary spasms like Prinzmetal’s.
One theory lies within the thin lining of the blood vessels called the endothelium. Usually this artery lining produces a chemical (nitric oxide) that helps to widen the blood vessel, allowing blood to flow through with ease.
But if the artery lining is damaged or isn’t working properly, the blood vessel may narrow and cause a coronary spasm. Levels of the artery-widening chemical are higher when estrogen levels are also high at certain stages of the menstrual cycle. A 2001 study published in the journal, Annals of Internal Medicine, suggested that during times when estrogen levels are high, women have fewer chest pain symptoms(3). In addition, smokers tend to have lower levels of nitric oxide in their blood vessels than non-smokers, and smoking is a major risk factor for coronary spasm.
Symptoms of angina can also occur in the absence of any coronary artery disease. Up to 30% of people with a heart valve problem called aortic stenosis, which can cause decreased blood flow to the coronary arteries from the heart, can have angina. People with severe anemia may have angina because their blood doesn’t carry enough oxygen. People with thickened heart muscles need more oxygen and can have angina when they don’t get enough.
We do know that cardiovascular disease kills more women than any other cause, about six times more women each year than breast cancer does, and in fact, more than all forms of cancer combined. Each year since 1984, more women than men have died of cardiovascular disease. Men tend to develop heart disease on average 10 years earlier than women do.
Anatomically, male and female hearts look about the same. When healthy, both should be about the size of a fist (a man’s heart is the size of a man’s fist, and a woman’s heart is smaller because it’s about the size of a woman’s fist). If you’re a woman, yours weighs about the same as a green pepper and, also like a green pepper, has hollow chambers inside.
Both men and women have three main coronary arteries surrounding their hearts. These are the large blood vessels that wrap around the outside of the heart, supplying blood, oxygen and nutrients to heart muscle to keep each heart pumping properly – and thus the arteries most susceptible to life-threatening cardiac events through obstructive – or non-obstructive – heart conditions.
But women who have a heart attack fare worse right after the event and also suffer a poorer quality of life.
Learn more about coronary microvascular disease:
- in this LA Times feature
- on this 22-minute video about identifying hard-to-catch diagnoses in female patients via medical imaging called Diagnosing Cardiovascular Disease in Women with cardiologists Drs. Redberg, Shaw and Bateman
- in this 5-minute video about my heart sister Joan Jahnke of South Carolina, who went to Emory Heart & Vascular Center to have her coronary microvascular disease appropriately diagnosed and treated
- on these websites from Mayo Clinic and the Texas Heart Institute .
♥
NOTE from CAROLYN: Please do NOT leave a comment here describing your current symptoms. I’m not a physician and cannot diagnose you online (nor can anybody else). If you are experiencing distressing symptoms, seek a medical opinion from your physician.
See also:
- Misdiagnosed: Women’s Coronary Microvascular and Spasm Pain
- No Blockages: Living with Non-Obstructive Heart Disease
- “I Rang the Bell Again. No One Came.”
- Coronary Microvascular Disease: a “trash basket diagnosis”?
- His and Hers Heart Attacks
- When Your Artery Tears: Spontaneous Coronary Artery Dissection
- The New Country Called Heart Disease

I have no blockages. I was admitted to the hospital with pain in my chest, back, left arm, left shoulder, neck and the right side of my jaw. I was in the hospital for four days. I went to a doctor’s appointment and was told that I had a cold that affected my heart and now it is all better. I still have mild chest pains, shortness of breath, fatigue, dizziness and bloating. Several months ago I had sharp chest pains and it hurt to swallow. My heart output (Ejection Fraction) was at 46% in the hospital and I was put on lisinopril for high blood pressure and Metoprolol to help my heart beat harder and increase its output.
My doctor said my dizziness was from low blood pressure and not to take the metoprolol. I am now searching for a doctor in the Atlanta area that will know what is going on with me because this one does not. I have had these problems for some time now and it just recently got worse. I fully expect to have another stay in the hospital since the Metoprolol has been discontinued. I fully believe that I have CMD and am grateful for this blog so now I know what is wrong with me and now can try to find someone to help.
Forgot to say that I had been to the Emergency several years ago with chest pain and was told it was acid reflux. This time they told me I was not having a heart attack, but they wanted to keep me overnight to start with. After a couple of blood tests they told me my enzyme level showed I was having a major heart attack. Now they tell me it was nothing.
LikeLike
Laura, I’m not a physician so cannot comment specifically on the many confusing issues you are describing here. I can tell you generally, however, that before any person takes not one but two drugs that lower blood pressure, it’s important to know for sure what your blood pressure is in the first place – otherwise, that doc who told you that your dizziness may be due to blood pressure that’s actually too low may be quite correct. Ditto with the importance of learning what all cardiac test results mean (your cardiac enzymes either indicate a “major heart attack” – or they don’t; ask for copies of your medical records so you can sit down with a physician and discuss all results). If something doesn’t make sense to you, ask questions. Do lots of homework based on credible resources (Mayo Clinic’s website is a good place to start). Know and track your numbers. Get a home blood pressure monitor, for example. Start a symptom journal (dates/time of day/activity levels) so you’ll have solid info to show your health care provider. And best of luck tracking down a doctor and getting some clear answers.
LikeLike
Laura, were your enzymes elevated? I was just in for the third time for NSTEMI. I hope you feel better! It is frustrating having a disease for which research is lacking.
LikeLike
My symptoms went on for a couple years, getting progressively worse. First a choking sensation, like someone had their hand around my throat. The muscles in my throat actually hurt as if they were strained. Thought thyroid, but no. This choking then became a pain which would spread down across my upper chest. As time went on this became more and more often until it was a daily event but now the pain would come starting in neck to chest, up the sides of my jaw to temples until I thought my face would explode. Icouldn’t bend over or pick up anything even taking laundry from dryer without starting to get tightness in my throat. Or course I had been to my Dr. I had a treadmill test with echo, all kinds of blood work, which said I was fine, actually had gone to emergency room three times with no diagnosis or heart problems, and yes I too was told ACID REFLUX! Which started the trek down that road. Had all tests and no acid reflux.
Then the night the pain refused to go away. Vomiting and perspiring. Now that got their attention. Imagine that, you must be sweating and puking to be having a heart, and in fact they were shocked to find the angiogram saw no blood in my heart. It looked like a ball of blood backed up and sitting atop my heart. Cath wasn’t possible. Heart too weak for surgery, so somehow a pump was placed in my heart for a full day till I was strong enough for open heart triple bypass surgery which the Dr couldn’t believe I survived. Now that was a real second chance from God. And I am so blessed. But my whole purpose for subjecting you all to this novel-length post is to say, please! Please! Please! Do not let anyone tell you that your throat disomfort isn’t heart related. Since my attack I tell everyone even drs not to poo poo a woman’s complaint about throat discomfort.
LikeLike
Hello Barbara – throat symptoms are commonly reported cardiac symptoms by women. So much of medicine is simply trying to rule out what the problem is NOT. But all unusual symptoms should be taken seriously. These may or may not be heart-related at all, but something is very wrong when you feel like your face might explode! My advice now to all women is this: You know your body! You KNOW when something is just not right. Pay attention to that little voice inside that’s warning you this is not “normal” for you.
LikeLike
Excellent! 🙂
LikeLiked by 1 person
Thank you for this article. I had an MI in 2011 with an added diagnosis of new onset Left Bundle Branch Block. LAD (left anterior descending coronary artery) was 50% blocked in 2011.
I never felt that I returned to my previous activity level following my heart attack at age 55. I am now age 58 and recently (August 13, 2014) had a heart cath which found my LAD (widow maker) 90% blocked. The cardiologist placed a stent.
It is now September 2014 and I do not feel any improvement in my symptoms. I continue to experience shortness of breath, chest pressure and fatigue. I have been researching my symptoms and am concerned that microvascular disease may also be present. I have a follow up visit with my cardiologist tomorrow and plan to ask for cardiac rehab and a follow up echo stress test to compare to the one done August 4, 2014, which I failed, the results after 3 minutes showed highly abnormal chest wall function…which led to my heart cath.
I am thankful that I found this site, I am not alone. I feel frightened, not just about the heart disease, but concerned about how I am going to be able to continue to keep working, keeping my medical insurance if I miss too much work, paying my bills. I am widowed and live alone. I do have some wonderful friends and two wonderful adult children who have offered assistance.
LikeLike
Oh, Michelle! I’m so sorry that you’ve been going through such a scary month. SOMETHING is causing these symptoms since your stent was placed last month, and you need to find out what. Asking for a cardiac rehab referral is a good idea as you need all the support you can get during this time (and why should patients have to even request this?!?) You might want to also ask about getting coronary reactivity testing – the preferred diagnostic test (as described above) for coronary microvascular disease according to the Harvard Health Letter. Good luck with your cardiologist’s visit tomorrow – between now and then, try to do as much reading and prep as you can so you’ll feel better informed when you discuss your options. And please let me know how it turns out, okay?
LikeLike
Thank you for your support Carolyn. My cardiologist shared with me the results and images of my heart cath and stent placement. I mentioned my ongoing symptoms and chest discomfort. He stated that it generally takes about five weeks to feel improvement after stenting. I asked if he thought I had microvascular disease, he replied that it was highly likely. No further testing was offered although I did get a referral to cardiac rehab. I see my primary physician this week and plan to request a referral to another cardiologist for a second opinion.
I love reading your blog Carolyn, I wish I had found your site years ago as I gain more information and insight regarding cardiac issues.
Thank you,
Michelle
LikeLiked by 1 person
Thanks for the update, Michelle. Sounds like you are now on a path towards further improvements. So glad to hear about your cardiac rehab referral. Please go (and complete!) that rehab – women tend to be cardiac rehab dropouts so DO NOT become one of those statistics! Meanwhile, keep reading and learning like crazy. As a wise nurse told me while I was still in CCU after my heart attack, “Your job now is to become the world expert in your particular cardiac issue!” Knowledge is power. Best of luck to you and thanks again for keeping us in the loop as you progress.
LikeLike
Hi Carolyn can you please tell me if “Coronary Reactivity Testing” is available in the UK
LikeLike
I don’t know, Linda. You’d likely have to ask this at a major cardiac hospital.
LikeLike
Reblogged this on Lit Salad and commented:
Don’t be afraid, but be aware.
LikeLiked by 1 person
Thanks for reposting this info on your blog, Beth!
LikeLike
ME. TOO! Same! Thanks for writing this.
LikeLike
You’re so welcome!
LikeLike
Great article. Several months ago at work, I had a backache for a bit, then felt faint.
I hadn’t eaten so thought that was the faint feeling. Food didn’t help. I did go to the Dr who said it couldn’t possibly have been a cardiac event because “you don’t have any risk factors.”
I am 10 years post menopausal, 60 years old. No EKG or anything was done. I now have a new job and an appointment with a new Dr.
I did “sneaky” EKG at work and seem to have U waves. “Uh Oh”. This time I will not take a pat on the head for an answer.
LikeLike
Cheryll – right now you don’t know if your odd symptoms were heart-related or not, but you did the right thing in seeking another opinion to help solve the mystery. Best of luck to you…
LikeLike
Cheryll, what do you mean by u waves? xx
LikeLike
I’m 54 who 2 years had 2 blockages in L.A.D (widow maker) It took a year to find this. Angina, repeated hospitalizations, stress test and echo normal, sent home to lose weight and calm down?
Stented in 2012 but within 2 months, angina back. BP spikes at all hours working or resting. After 5 ER visits and overnight stays, switched Cardiologist. 1st visit flunked my 1st physical stress test. ER visit followed that with overnight then chem stress test, flunked that too. Cath done the next morning. In this, lesser vessel found with 95% blocked but other vessels forming to take care of the block.
They say all the gunk from L.A.D was pushed in to vessel when stent was placed. To fix this vessel would compromise stent (they don’t want to do this).
So now I’m waiting for a LITTLE heart attack. Don’t know when? Angina is worsening, short of breath, and all that goes with this. I can’t work, am filing for SSD. (Ha Ha). Ticking time bomb. Meds are always carried. I know where all hospitals are when out and about (just in case).
I’ve spent since Jan 14 trying to find info on this. This site is the best. I’ve gotten more info here then all the searching I’ve been doing.
My question is does this sound right? 7 Cardio’s since this started. The one that did stent moved out of my area so it’s taken me several Docs to find this one that actually found the problem. I will be anxiously watching for any comments!
LikeLike
Hello Cat and thanks for sharing your story here – definitely NOT a textbook case, which is why you’re overwhelmed with symptoms that don’t respond politely to treatment so far.
I’m not a health care provider, so can’t comment on your specific case, of course, but I can tell you in general that you should be seeking immediate help for any angina that you describe as “worsening”. Since you mention “meds are always carried”, I’m guessing you’re on nitro tabs/spray. Has your doctor mentioned if a nitro patch is appropriate for the amount of angina you’re experiencing? What is your doctor’s plan to manage those BP spikes? (You’re right – losing weight and staying calm might very well help that).
Here’s what I’m concerned about: your description of “waiting for a heart attack” and “feeling like a ticking time bomb”. That kind of low-grade chronic stress and anxiety – while perfectly understandable! – in itself is NOT good for your heart, as you already know. And wasting precious hours you’ll never get back by waiting for a heart attack that may not happen is exhausting and futile. Please consider your local Pain Clinic, or seek professional therapy to help you manage, learn about Mindfulness Meditation or Relaxation exercises you can do on your own, and if you haven’t gone to Cardiac Rehab, ask your doctor for an immediate referral. Waiting for your disability application to be processed is in itself a terribly stressful experience – so while you’re waiting, please do whatever you can to reduce that stress (no matter how worried you are about it, it simply won’t affect the outcome).
And how about keeping a symptom journal to document what symptoms hit, when, what you’re doing when they do happen, or what you were doing just beforehand. That way, you’ll have comprehensive documentation to help your cardiologist help you. When I track my chest pain due to coronary microvascular disease like this, I’m sometimes surprised to find that what I’d been describing as “non-stop” angina turns out to be far less frequent than I’d thought.
Your challenge now is to become the world expert in your unique condition. Best of luck to you.
LikeLike
So what about if you feel like there is knot between your shoulder blades that is causing a lot of discomfort and even after you get your husband to massage it, it does not feel any better, or if you feel a lot of discomfort kind of like heart burn but you feel full and then become very gases and it is burning?
LikeLike
Seek medical help.
LikeLike
Lee, I cannot speak to reflux, which is what the second half of your comment sounds like, but If I may make a suggestion to try? I also have MVD/CMD of many years and lived with that “knife in the back”. I was referred to a certain kind of physical-therapist by another physical-therapist. The second one was trained first in “Rolfing”, but more importantly, in something called the UPLEDGER technique and the Baral or Barral technique. This is a body work approach that concentrates on the abdomen and chest/back (core) and seeks to subtly find and release fascial tension surrounding the organs. If you can visualize the silvery skin surrounding a muscle if you have trimmed a roast, then know that that is the “fascia”. It can constrict and carry pain signals as much as muscles. When you release the muscle through massage, it does not also release the fascia.
This therapy approach allowed the therapist to “reach through” the muscles of the chest, back and diaphragm, and release the fascia that surrounded my lungs/heart and who knows what else. All I know is this: after my 2 hour session, the knife had been removed from my back.
The way I view it is this – ischemia and hypoxia to the tissue, INCLUDING the FASCIA, is a chronic body response when we have heart issues. That fascia has no way of unwinding itself from a tightened state. I’d had cumulative tightening for many years. When she worked on me – it released. I can’t quite describe the relief I had when this happened, and it is now almost 6 months, and it has not returned.
I have since gone to her for other back and neck related issues, but I will make having a tune up for my “knife” a priority, should it reappear. Try searching the internet for those terms/techniques.
All the best ~
LikeLike
80% of heart attacks occur in arteries less than 70% obstructed by the blockages we call plaques even though there is still no reduction of overall blood flow.
LikeLiked by 1 person
My mother had a blocked left coronary artery, +90% and evidence of a prior major heart attack, suspected to have happened the prior August, over a year before her death.
This was discovered during an autopsy. My father and I hired an independent forensic pathologist. One of the first things he said when I was describing all her symptoms and especially jaw pain..her face and jaws would litterly pulse.
She had had multiple espisodes of leg swelling, right sided weakness, near loss of concsiousness…went to emergency a number of times. In fact, 4 of the major hospitals in Seattle! None of them diagnosed or suspected her heart. One of her doctors even told me when I wanted pulmonary testing done, “I think it’s more psychosomatic”.
LikeLiked by 1 person
Lynn, in your mother’s case, her heart attack WAS evidently caused by a blocked coronary artery, but the concern is that current diagnostic tools were unable to accurately identify that blockage before she died. A tragic situation.
LikeLike
I’m female, 51 and one week ago (12/13/10) experienced an 80% blockage to the Left Anterior Descending Coronary Artery – “Widow Maker”.
I had never heard the term until my Cardiologist stood over my bed and said you had a widow maker blockage. I was shocked. Over the past 3 months, I had experienced a host of heart attack symptoms (Palpitations, left arm pain, neck pain, jaw pain resembling a toothache, wheezing when I breathe, and finally massive chest pain which I still thought was gas (indigestion) but did not put together the connection.
It is important for women to be their own health care advocates. I had x-rays of my left shoulder and arm and was seeing a chiropractor for the pain in my neck and back. I attributed my tiredness to a diagnosis of fibromyalgia. I was scheduled to see the dentist for my reoccurring tooth pain on the day I had my emergency heart catheterization. I did everything I knew which included reporting my symptoms to my Doctor but she never connected the dots – and for that I could have died.
LikeLike
i live in Ottawa and cannot find any help for my cardiac syndrome x. the doctors here are ignoring me and treating me like im crazy. can anyone help.
LikeLike
Hi Teresa – in Ottawa, you have access to the University of Ottawa Heart Institute (meaning more cardiologists per square inch than most other cities) but more importantly, your biggest role is that of being your own best health advocate. Cardiac Syndrome X and microvascular disease are challenging diagnoses. Research as much as you can – print off the Mayo Clinic and Texas Heart Institute references above and bring them with you to every doctor’s appointment. We also know that inflammation and smoking are now considered contributors to this diagnosis. SOMETHING is causing your symptoms and you need to be tireless in demanding appropriate care and treatment. Good luck to you.
C.
LikeLike
Hi Carolyn,
I’ve brought in articles* from Dr. Noel Bairey-Merz who kindly mailed me her own research articles when I told her the doctors at the Ottawa Heart Institute were refusing to listen to or help me. I spoke with one of her colleagues on the phone about the tests I’ve had, the results, my symptoms and she said that I meet the criteria for diagnosis of microvascular disease i.e. persistent chest pain, abnormal perfusion test, and normal angiogram. I told her what my cardiologist said to me: “It’s impossible to have a heart attack and that it’s not a serious medical condition” – and she told me he is wrong.
I went back to the hospital and told them what Dr. Bairey-Merz’s colleague told me, brought in the research articles and they are refusing to adjust my cardiac meds. My sense is that in Ottawa this disease and the needs of women when it comes to heart disease are ignored; not only this, but women with true cardiac conditions are labelled as crazy if they try advocating for themselves.
I was told by a resident from the Ottawa Heart Institute that in Ottawa 50% of the cardiologists “don’t believe in Cardiac Syndrome X at all” and he said good luck in trying to find someone with an open mind. He also said that in Ottawa, they have no test to diagnose Syndrome X directly. Because of this it tends not to be diagnosed accurately, and honestly as a woman with this disease, I don’t know where to get help?
What I don’t get is that each year the Heart Institute goes to the public and says we need money for research to fight heart disease, and yet in 2006 sound research came out about microvascular disease that they are ignoring.
As well, in 2007 the Heart Institute told me that they have no test to diagnose Cardiac Syndrome X. It’s now almost 2012. Why haven’t they purchased the technology? (functional angiography or specialized MRI). They have it in the States. Why is not available here, or then why aren’t women sent to get the test across the border?
It seems like they only care about men. They will not adjust my meds because they have no test, even though when I was diagnosed they said my meds would be adjusted as needed.
* For example: Reis SE, Holubkov R, Conrad Smith AJ, Kelsey SF, Sharaf BL, Reichek N, Rogers WJ, Bairey Merz CN, Sopko G, Pepine CJ. “Coronary microvascular dysfunction is highly prevalent in women with chest pain in the absence of coronary artery disease”: Results from the NHLBI- sponsored WISE study. American Heart Journal 2001;141:735-41.
LikeLike
Hello again, Teresa. I hesitated at first to publish your long story about your experiences with the OHI, but ultimately decided that yours is unfortunately such a common experience for so many undiagnosed women – in Ottawa and elsewhere! – that it may be worth rattling some cages. Dr. Bairey-Merz of Cedars-Sinai Medical Center in Los Angeles is widely considered a credible expert on the subject of Coronary Microvascular Disease. Here’s how the Harvard Heart Letter editor recently described her take on MVD:
“The gold standard for detecting microvascular disease is currently coronary reactivity testing. This angiogram-like test lasts 60 to 90 minutes and allows doctors to see how very small vessels supplying the heart respond to different “challenges” from medications. Showing slides of tiny vessels that narrowed in response to a certain drug when they should have widened, Dr. Bairey-Merz emphasized that microvascular disease is not a benign condition, as previously thought. “This is real ischemia,” she said.” Here’s more from Harvard (Dr. Bairey-Merz’s alma mater, coincidentally).
I’ve just returned from attending the 46th Annual Canadian Cardiovascular Congress in Vancouver, where I was truly dismayed to discover that, out of over 700 scientific papers, only a tiny handful focused specifically on women’s heart disease risk factors, diagnostics or treatments.
When it comes to heart disease, it does indeed still appear to be a man’s world out there.
LikeLike
Dear Carolyn,
As a registered nurse who practices in the province of Ontario, I was dismayed by the exchange of letters between yourself and Teresa.
Like you, I have just returned from Vancouver after attending the Canadian Cardiovascular Congress. It is clear that continued research is needed in the field of Women’s Heart Disease and there is a strong need to continue to advocate for access to care.
As nurses we have a clear mandate to advocate for patients and help them achieve their optimal level of health.
I wonder if Teresa might benefit from contacting a Regional Cardiac Care Coordinator working at the Ottawa Heart Institute to help her continue to advocate for herself and access care.
Regional Cardiac Care Coordinators (RCCC) are registered nurses that work in Ontario hospitals offering advanced cardiac services. They have a variety of roles, one of which is to provide education and support to patients and families and play a key role in helping patients and families navigate through the health care system during the waiting time for advanced cardiac services and facilitating the patient care from booking until discharge. Their function is an extension of the role that the Cardiac Care Network (CCN) of Ontario plays in the delivery of advanced cardiac care in the province.
Teresa can learn more about CCN and the role of the RCCC. Or contact a RCCC here.
Teresa may also find the following website helpful – although it does not specifically deal with cardiac issues there is some information around current initiatives.
All the best Teresa, and please let us know how your journey progresses.
Paula Roberts
LikeLike
Thanks so much Paula for this helpful information. Ontario’s Cardiac Care Network sounds like a groundbreaking role model for all health care systems. However, its utility in helping heart patients to navigate the system is focused on patients who already have a diagnosis. That seems to be Teresa’s dilemma: she has been unable to get a clear diagnosis yet. I’m hoping that she does, however, follow up with the links you provided here.
We live in hope!
Cheers,
C.
LikeLike
Dear Carolyn and Paula,
Thank you for your interest in my comments. Paula, I have read the links that you provided concerning equity and womens health as well as the role of the CCN and RCCC. Right now there is inequity in the health care system in its delivery of cardiac care in favor of men and this is why.
Very sound research came out in 2006 called the W.I.S.E. study which found that how heart disease is diagnosed and treated is flawed in favor of men and this was because what we knew up to that point was based on research which only studied men.
Symptoms in women are different, their hearts are different, women may need different diagnostic testing because standard tests miss heart disease in women, and the way that women develop heart disease can be different than in men. And also the way cardiologists determine severity of illness is also flawed in favor of men.
All this is to say that we need to implement this new evidence now so that women can get the help they need, and to me as a woman and patient on the ground utilizing the system, knows it’s not working, it’s not equitable.
There are barriers from start to finish in the health care system when it comes to heart disease from at first when women’s symptoms are labelled as “atypical” (and/or emotional, gastric), to the EKG, stress test and angiogram which miss microvascular disease, to the EKG and stress test when abnormal is interpreted by the cardiologist as “false positives”, to the angiogram done after the abnormal stress test which is normal and the woman is told nothing is wrong with her heart, to the woman who is finally diagnosed with cardiac Syndrome X and is told it’s a benign condition because there is no access to proper testing or expertise and she is not sent anywhere because her symptoms or condition are not serious, or she is denied access to the proper medical management of her condition because of lack of expertise or testing.
All this needs to change. I’ve read what was provided concerning the role of CNN, however I see a potential problem because it’s based on a doctor’s opinion which is being formed within a system which is flawed against women and herein lies the entire problem.
LikeLike
Hi Teresa,
I have been having severe chest pain. I ended up in the Emergency room 3 times.I was told all my tests were negative & sent home. I was recently investigated at the Ottawa Heart Institute. I was told that there is nothing wrong with my heart but that my pain is due probably to fibromyalgia. I have requested another appointment with the cardiologist at the Ottawa Heart Institute because of this debilitating chest discomfort, pain in the left arm, pain in the jaw that is not going away, but my request was denied.
My family doctor said that he was happy that the Ottawa Heart Institute didn’t want to see me again because he said they were the EXPERTS so not to worry about my heart. He is considering treating me with an anti depressant medication!!!!!! The pain makes me very anxious at times but I hate being treated that there is nothing wrong with me!
Now that I have read your story, I am going to fight. First I am going to print off all the information’s from the Mayo Clinic & Texas Heart Institute & bring copies to my family doctor & mail some to my cardiologist at the Ottawa Heart institute. Hope they hear us before it is too late… Good Luck
LikeLike
Hi Claire and Carolyn,
Although this is really good information and a good site, sadly I have to say that the cardiologists in the Ottawa area in my opinion ignore microvascular and prinzmetal’s disease.
There is no testing that I’m aware of for either. I’ve already said this before but to reiterate my experience, I was diagnosed with cardiac syndrome x and angina, at the Civic Hospital following an abnormal PET scan which showed lack of perfusion and scarring in the heart muscle. However later at the Heart Institute, who your doctor refers to as THE EXPERTS, my diagnosis was changed to “presumptive cardiac syndrome x” because they said the PET scan is only an indirect test and they don’t have a direct one. After I was diagnosed, my husband and I asked to be referred to an expert in cardiac syndrome x because we felt the cardiologist didn’t know very much about the disease.
We were told there is no one. After the diagnosis I was told that my heart is “normal” and if I do have cardiac syndrome x – it’s not serious – it’s a benign condition, while other doctors at a different hospital told me that if my angina is not treated that it will lead to a heart attack.
I feel that the doctors perhaps pay more attention to things where the science is more solid or they have the tests to be sure. People with these conditions unfortunately don’t get the right kind of help they need and their chest pain is often left undiagnosed, misdiagnosed and left untreated.
I don’t know why they ignore these diseases? They don’t in the States. Do Canadian women not deserve to have their chest pain treated – PROPERLY? Honestly, I feel that it poses more of an economic burden on society and the health care system when doctors don’t diagnose their patients in a proper and timely way in the first place. These patients get sent to a lot of different specialists that they don’t really have to see – which costs more money in the long run, all the while the patient becomes sicker and more of a burden on society as they are able to do less, and later if they are finally diagnosed the cost to treat them is more than if they had been diagnosed the first time they experienced their symptoms.
The doctors at the Heart Institute should be honest with the public. We rely on their integrity and expertise. If they don’t really know and aren’t really sure, they should say this to the patient and their family doctor and not send them on wild goose chases and stop pretending.
In Claire’s case for example, they could say in the report to the family doctor that it could be cardiac syndrome x. Since they have no tests to diagnose this condition properly, they should have her come back if her symptoms worsen. They told me they can only diagnose cardiac syndrome x by paying close attention to the symptoms and using their clinical judgement. Claire describes her pain in her chest, left arm and jaw. Although I’m not an expert, to me that sounds more cardiac than fibromyalgia. Or they could have her try pain medication when she gets the pain to see if it subsides. I know in my case it was only when Dr. Wong put me on Atenolol, a cardiac drug, that my chest pain disappeared, but for the cardiologists at the Heart Institute in my case that’s not enough to convince them. They will only be convinced by absolute proof, yet they will not find me the test I need because after all in their opinion microvascular disease is not that serious.
LikeLike
Teresa and Claire,
This recent podcast appeared on a cardiologist’s web site. If a cardiologist is dismissive after listening to this (you can lead a horse to water, but…), then I don’t know what to tell you. Keep searching for a doctor who is open to new scientific information!
LikeLike
I live in the USA. I had been misdiagnosed by over 10 cardiologists and 8 PCP’s. Unlike Canada, I was billed for every person I saw with a $16,000 deductible on my heath insurance. From May 2012 to Dec 2012, I had a heart attack, 2 stents put in, and had to go from Moscow, Idaho to Spokane, Wa to Tucson, Arizona and to Lewiston, Idaho and Coeur d’alene, Idaho.
All the bills not paid by my husband’s insurance and we were sued for unpaid medical bills that bankrupted our family. We have sold everything but our home, and we are praying on a miracle to save our home. None of the cardiologists would sign a release for me to go back to nursing and told me with time I have left to file for disability.
The health insurance in the USA is horrible and will bankrupt the middle class person. I was treated as a delirious drug seeker even though I had an excellent reputation as an honest outstanding nurse. I was sent home with angina so bad I could not walk and told it was all in my head after I had been diagnosed by a cardiovascular specialist in Seattle for severe microvascular cardiac disease with unstable angina and apical ischemia.
I don’t know what tomorrow brings but I have to die at home.
I have 4 insurances with deductibles and copays I cannot pay. I have no money for groceries meds or gasoline. Ruined in America by this debilitating disease.
LikeLike
A tragic story, Veronica. I wish I knew what to say to help you. Best of luck to you and your family.
LikeLike
I am forty eight and also experienced a 99% blockage in the big left anterior descending coronary artery – the so-called widowmaker heart attack, with no other blockages in any other arteries. I do have a stent. I have no family history, do not have high blood pressure, diabetes or high cholesterol. I am an interval jogger, jogging 12-16 miles a week, but am overweight.
This has taken me by surprise. I understand that stress could be the only other risk factor. How does stress affect the body? What is the likelihood that I could experience another?
LikeLike
Hi Lorrie and welcome to the very exclusive club that none of us ever wanted to join! Yes, there is a growing body of evidence linking chronic stress with cardiovascular disease. For more info, see: “Women’s Heart Disease and Chronic Stress” which includes helpful links to the world-famous Cleveland Clinic (considered the #1 heart institute in North America) offering strategies for managing stress to improve cardiovascular health, as well as a link to a ‘Yoga Journal’ article on how your response to chronic stress can contribute to your overall heart attack risks.
Nobody can predict the likelihood that you’ll experience another heart attack, but the reality is that heart disease is chronic and progressive, and even though they can patch us up, stent us, bypass us, defibrillate us – medical interventions do not address what caused that coronary artery damage in the first place. We also know that heart disease is 20-30 years in the making.
My observation so far has been that while there are often clear risk factors to explain cardiac events, there are also those patients who seem to defy the odds and develop heart disease without apparent risk factors. But you WILL be on the right track if you are aggressively making diet, exercise and stress-reduction lifestyle improvements now. Good luck…
cheers,
C.
LikeLike
The inner lining of a healthy artery is very smooth and allows blood to flow freely. As plaque buildup progresses, it will accumulate calcium deposits, and this makes the artery stiff and hard. It also roughens the inner surface of the plaque, causing turbulence in blood flow in the area of the plaque. With time, the lining of fibrous tissue over the plaque may be eroded by this turbulent flow, and the inner core of the plaque is exposed to the blood stream. When this fatty core is exposed to blood a thrombus (blood clot) may form. This may cause the blood vessel to suddenly become totally blocked, a condition known as thrombosis. When this happens in a coronary artery, there is a sudden decrease in blood flow to heart muscle which causes a heart attack or myocardial infarction.
LikeLike
This was interesting because I have also had both diagnosises. I had a 90% blockage in the LAD and also have microvascular disease. Thanks for the article.
LikeLiked by 1 person
Thank you for this, Carolyn. I was recently diagnosed with Prinzmetal’s Angina after over a year of “normal” cardiac tests and increasing frustration and despair at being blown off by doctors who figured I was just a middle-aged menopausal hypocondriac (sp?). No blockages, just spasms of the coronary arteries, and it’s treated with medicines, not surgery or stents.
Why don’t more doctors know about these kinds of non-obstructive heart conditions in women?
LikeLiked by 1 person
Very interesting. I will read more about this, as I also had the widowmaker and want to know why and what really happened as it has never been explained to me.
I also want to know about rate of recurrance and prevention.
Thank you,
Chris
LikeLike
Hi Chris,
This Mayo Clinic website has lots of info that may answer some of your questions about preventing a second heart attack.
Stay well!
cheers,
C.
LikeLike
Why is it that doctors do not explain why it happens? I am a 50 year old female, I thought I was in great shape, I too had the widow maker and no doctor has told me why. I just switched cardiologists, and this was the main reason why. I need a doctor that will sit down with me and explain what went wrong and why!
LikeLike
Hi Laureen – it’s important to keep in mind that sometimes there is no clear answer to the “why” question. If there were, your doctors could easily answer that question. Sometimes, nobody can know exactly why. Your job now is to become a ‘world expert’ in your condition, and that includes becoming educated about all cardiac risk factors. Best of luck to you on this journey.
LikeLike
I am 32 and had a 100% blockage in my RCA. I had 2 stents placed. A month later chest pain again and was re-cathed; was found to have smaller than normal arteries and 40% and 60% blockages in other arteries no stents placed that time. So now I just wait like a ticking time bomb!
LikeLike
Hi April – you are very young to have experienced these cardiac interventions. Please try not to focus on that “ticking time bomb” visual – it’s a very unhealthy and non-productive way to spend time ruminating. As a general rule, the clinically accepted medical criteria for stenting do not recommend revascularization procedures unless coronary artery blockages are greater than 70%. I hope you were referred to a cardiac rehabilitation program after your last procedure – we know that regular exercise programs can improve heart function.
LikeLike
Hi April, my name is also April and I had 90% blockage of my LAD 2 years ago when I was 38 years old. They could not stent it because it was at the truck of the bifurcation, so I ended up having to have an open-heart single bypass. After recovery I started exercising again and getting back to normal as much as possible. A few months ago I was having horrible heartburn that would not leave so they kept me all night in the ER and ran multiple blood tests that were normal. The next morning they did a nuclear and physical stress test which was slightly abnormal so they set me up to do another catheterization. The doctors said my bypass looked good and my other vessels looked good too. Well yesterday I was doing my normal cycling class and was probably overexerting myself a little and all of a sudden had a horrible sharp chest pain on the left side of my chest that stopped me in my tracks. Then I started to get a little nauseous so I got off the bike, sat down, and took a nitro tablet. When I got home I took an anxiety pill and made sure to take it easy the rest of the night. I don’t know if I should have gone to the ER or not, but I had a horribly stressful weekend (especially the night before) because my husband and I were having an argument about something, so I am really thinking it may just have been stress related since my blood pressure was probably way up the night before.
I called to talk to a cardiac nurse today just to see what they think just in case, waiting for a call back. Hate to rush in and feel stupid about it being nothing, but scared me a little bit. Now that I have read this article I wonder if I might have something similar going on. I feel your pain about being young and having these crappy problems, hang in there and take care, you’re not alone 🙂
LikeLiked by 1 person