 .This is a man told by the photographer to act like he’s having a heart attack.
.This is a man told by the photographer to act like he’s having a heart attack.
by Carolyn Thomas ♥ @HeartSisters
One of the reasons that I knew I wasn’t having a heart attack (even while I was actually having one) was my very inaccurate stereotype of what a woman’s heart attack can look like.
I used to think that heart attacks happen only to men. Old men. Mostly out-of-shape chain smokers and heavy drinkers. Old, out-of-shape, smoking, drinking men, who one day out on the golf course suddenly clutch their chests in agony and keel over, unconscious. CPR. 911. Golf buddies yelling. Ambulance sirens. Paramedics. Defibrillator paddles. That’s a heart attack, right?
Wrong, my dear heart sisters. That’s NOT a heart attack.
There is such an event, and it’s called sudden cardiac arrest. The surprising truth is that, while sudden cardiac arrest is an extreme medical emergency, it is not a heart attack.
A cardiac arrest is more like an electrical problem that causes the heart to stop beating and lungs to stop breathing. A heart attack, on the other hand, is more like a plumbing problem. It happens when the blood supply to the heart muscle is slowed or stopped because of a blockage or spasm in one or more coronary arteries, but the heart does not stop beating (unless the damage to heart muscle is so severe that a fatal arrhythmia – an electrical misfire – happens, triggering sudden cardiac arrest).
Women’s heart attack symptoms can range from severe to vague – and everything in between. Chest pain is the most common heart attack sign in both men and women, but remember that many women may not even use the word “pain” to describe chest symptoms (often replacing that with words like heavy, pressure, dull, ache, fullness, etc.) Depending on which research study you find, between 10-40% of women report NO chest symptoms during a heart attack. Every woman is different, of course, but here are just some of many symptom options:

Now, here’s why I suspect that those dramatic yet misleading cardiac arrest photos are dangerous: if women mistakenly think that a “real” heart attack is one that always looks like that guy and his buddies (because almost all media articles we see about heart attacks feature pictures that look just like him), we may not believe our own symptoms are heart-related at all.
So if you’re an editor or journalist writing about heart attacks, please learn the differences between these two distinct conditions and advise whoever is picking out images NOT to use photos of men in mid-cardiac arrest. (As a former journalist, I understand that reporters rarely if ever write their own headlines or choose their own images, but somebody at your media outlet needs to start educating those who make those decisions, so it might as well be YOU).
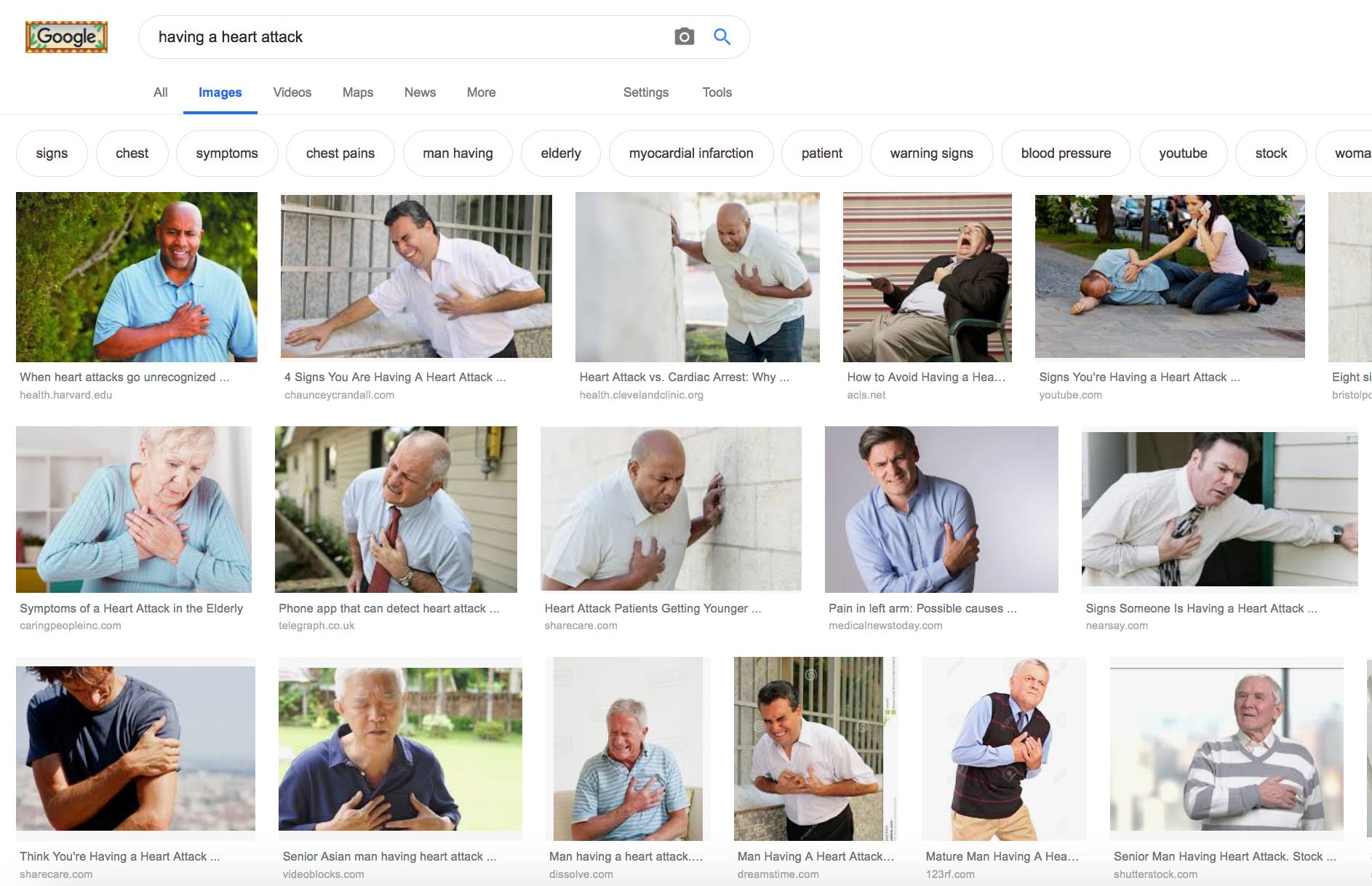
Just for fun, I Googled “having a heart attack” while drafting this article. Here’s but a small sample of the images that came up in my search, with pix of men vastly outnumbering those of women. This may help to explain why a Women’s Heart Alliance survey found that less than 45% of women recognize cardiovascular disease as the number 1 killer of women.
During my own heart attack, I could walk and talk and think and drive my car and go to work and fly to Ottawa over a number of days, all while suffering increasingly debilitating cardiac symptoms that came and went and came back again, continually. Researchers call this the “slow onset heart attack“.
I believed the Emergency physician who misdiagnosed me and sent me home despite my textbook Hollywood Heart Attack symptoms of central chest pain, nausea, sweating and pain radiating down my left arm. (“You are in the right demographic for acid reflux!”, he pronounced confidently).
And no wonder I believed him. After all:
- my symptoms weren’t what I believed “real” heart attack patients have
- I would much rather have indigestion than heart disease, thank you very much!
- he had the letters M.D. after his name and seemed very sure of himself
- his nurse colleague came up to my bedside at one point after he had moved on to the next patient in Emergency, and warned me quite sternly that I’d have to stop asking questions of this physician, adding:
“He is a very good doctor, and he does NOT like to be questioned.”
The question that I’d just had the temerity to ask the doc?
“But doctor, what about this pain down my left arm?”
I could not get out of that place fast enough!
I left feeling so horribly embarrassed because I’d just made a big fuss over “nothing” that, when my symptoms returned, there was no way I was going back to that hospital for help. That is, until my “acid reflux” symptoms finally became unbearable. That’s when I forced myself to return to Emergency – this time to a different doc and an appropriately correct cardiac diagnosis and immediate urgent treatment.
If somebody had taken a photo of me to illustrate what a heart attack looks like during the days leading up to that correct diagnosis, it may have shown me sitting at work with sweat dripping off my nose onto my desk blotter, popping Gaviscon like candies. No clutching my chest. No sliding off my chair, unconscious. No drama. Just feeling really, really dreadful.
At one of my recent Heart-Smart Women talks, one of the audience members asked me:
“What might you do differently if you had a chance to replay your first visit to Emergency?”
I told her that the most dangerous decision I made back then was deliberately choosing to ignore my worsening “acid reflux” symptoms.
So instead of standing up for myself, I meekly left the hospital that day feeling embarrassed, humiliated and clearly too stupid to know the difference between indigestion and a heart attack. But I also felt relieved that it wasn’t my heart, because I knew that my own symptoms didn’t feel like “that guy” (e.g. clutching my chest in agony and falling down).
I will never forget the heart attack survivor I met during my Mayo Clinic training who had also been misdiagnosed and sent home from Emergency. But unlike me, she kept going back to her local Emergency Department, despite being misdiagnosed each time. During her return trips, she insistently told the staff: “I know my body! SOMETHING is wrong with me!” At her third desperate trip back, she was advised to consider taking anti-anxiety drugs. At her fourth visit, she underwent emergency double bypass heart surgery.
Even the name of my particular type of heart attack still has a male name: the widowmaker heart attack. They don’t, for example, call it the “widowermaker” when women like me survive this.
Isn’t it about time we stopped giving it a male face, too?
.♥
Q: Would you prefer to see fewer pix of men in agony out there to illustrate women’s heart attacks?
NOTE FROM CAROLYN: I wrote much more about cardiac symptoms (all kinds!) in Chapter 1 of my book, “A Woman’s Guide to Living with Heart Disease”. You can ask for it at your local bookshop, or order it online (paperback, hardcover or e-book) at Amazon, or order it directly from my publisher, Johns Hopkins University Press (use the JHUP code HTWN to save 30% off the list price).
See also:
What sudden cardiac arrest looks like
Slow-onset heart attack: the trickster that fools us
Finally. An official scientific statement on heart attacks in women
How can we get female heart patients past ER gatekeepers?
Let’s pretend that atypical heart attack symptoms don’t exist
How does it really feel to have a heart attack? Women survivors answer that question.

Did that doctor and his nurse colleague ever find out that you actually had been having a heart attack? I hope so, for the sake of humility, not humiliation, though perhaps they deserve that, too. A good humbling now and then can do wonders in the path to improvement, and I’d hate for them to make the same mistake.
LikeLiked by 1 person
Hi Julie – I don’t know if that ER doc or the nurse ever found out. I’m guessing “no” because there is no such thing as mandatory reporting of diagnostic error. Medicine is apparently unique among workplaces in that when something bad happens, everybody agrees it’s best not to mention it again…
I did tell the ER staff and cardiologist that I’d been to this same ER two weeks earlier but had been sent home with an acid reflux misdiagnosis, but there’s no requirement for those people to officially notify anybody (their supervisor, the chief of staff, the hospital lawyer…) that this patient had been admitted and treated appropriately for a heart attack that had been missed by other staff members.
When the National Institute of Medicine issued its landmark report on misdiagnosis a few years ago, the chair of the report committee said (TWICE! during the media launch in response to reporters’ questions): “Now is not the right time for mandatory reporting of diagnostic errors.”
If the field of medicine were, like every other workplace out there, serious about public safety, you can bet that every incident of medical error or misdiagnosis would be recorded, discussed at rounds, taught in medical schools. You simply cannot fix something that is not measured – never mind talked about!
Scenarios like mine are considered ‘close calls’ or ‘near misses’ because I did not die. Had I died, there MAY have been some investigation IF my family had demanded an investigation… I wrote more about that craziness here.
LikeLike
Silent killer heart attack can happen to anyone. Thank you for us such a broad explanation of what women’s heart attack looks like. A heart attack is when blood flow to the heart is blocked, and sudden cardiac arrest is when the heart malfunctions and suddenly stops beating unexpectedly. Very dangerous.
LikeLike
Dangerous indeed, Gregory…
LikeLike
When in extreme, continual, and unusual (for you) pain, and told, “It’s nothing,” because of Hysterical Woman Syndrome:
Remove the image of physician as God.
Get another medical evaluation from a different doctor.
THANK YOU. Lessons learned.
LikeLiked by 1 person
Hi Sharon – good reminder for all of us: a second opinion is almost always an option, and our right. Nobody living with “extreme, continual, and unusual (for you) pain” should be told ‘it’s nothing’ because it clearly is NOT nothing…
LikeLiked by 1 person
The knowledge you have been sharing through this post is very much helpful. Thanks for sharing this post.
LikeLiked by 1 person
I too used to picture a heart attack as portrayed in the news by (older, male) patients, not by people who look like me. And my symptoms came and went over several days each time coming back more severe but the fact that in between I could drive my car and shop for groceries and visit with friends convinced me that, whatever was causing my symptoms could not possibly be a heart attack right? So I didn’t call my PCP or go to the ER right away because I “KNEW” that I didn’t look like the men in this post.
I never knew how wrong my “stereotype” was until I was finally hospitalized after the cardiologist told me that it’s not unusual for women to experience symptoms that come and go, and also that the worse symptoms do not necessarily mean a worse heart attack. Sometimes a woman’s symptoms can actually be quite mild like having the flu, the so-called “silent” heart attack.
All women need to know about these facts.
LikeLiked by 1 person
Hello Po’L – it’s hardly surprising that if we see only (older, male) heart attacks portrayed in the media, we learn that this must be what all heart attacks look like. As you say, you knew you didn’t look anything like those men in the media photographs you’d seen all your life… You probably looked more like a WOMAN having a heart attack – an image that’s much different than clutching your chest in agony and falling down unconscious.
Which is why editors and journalists must choose heart attack images that aren’t limited to men.
LikeLike